Inspired by Patients “To Remember”
Age is the most significant risk factor for developing neurodegenerative diseases that affect key brain functions like cognition. As the global population ages, the prevalence of neurodegenerative diseases is growing. Disorders like Alzheimer’s, Parkinson’s and Multiple Sclerosis result in disability and death of millions of patients around the globe and incur nearly $1.5T annually in health care costs in the EU and US alone.
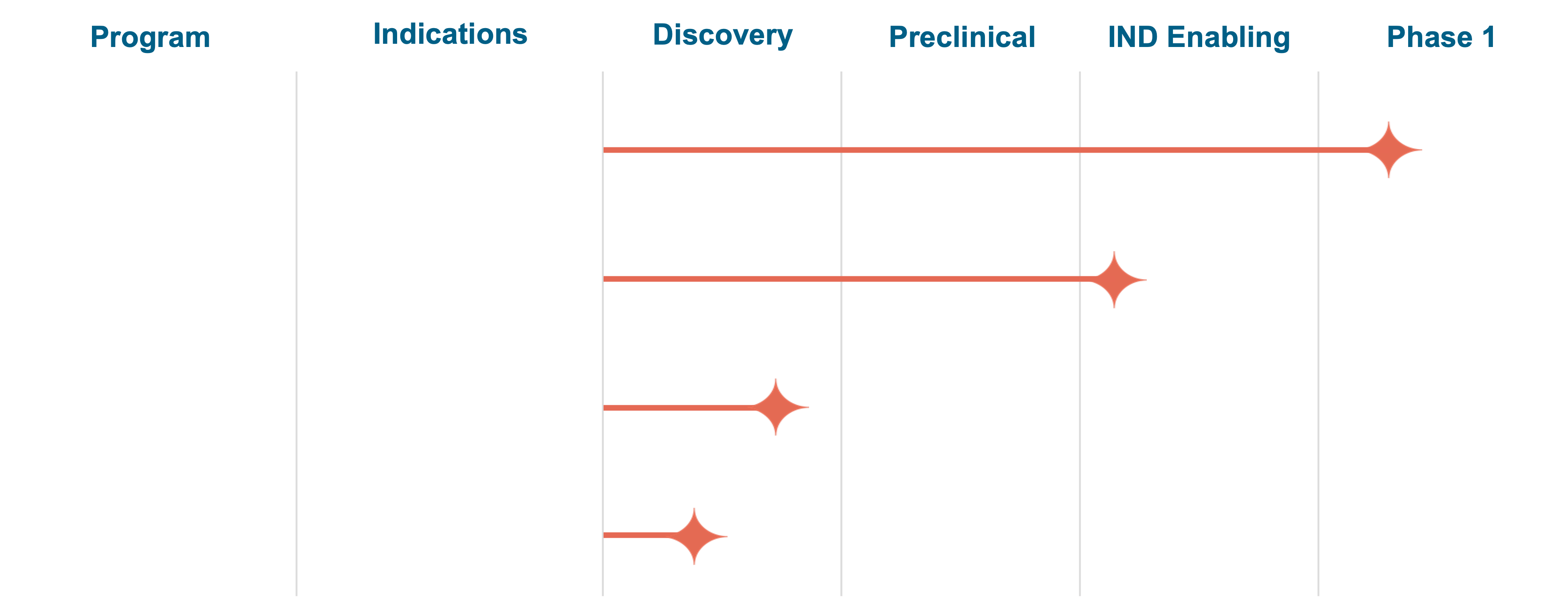
Muna colleagues work tirelessly to discover and develop disease modifying small molecule therapies for disorders that impact memory, movement, language, behavior, and personality. We transform groundbreaking science into life-changing therapies that preserve cognition and other brain functions and enhance resilience to neurodegeneration. Our name reflects our focus on preserving key brain functions, like cognition, so patients can live their best lives: Muna means “to remember” in Old Norse.